Chapter 2
Background
Introduction
2.1
Both Mr Percy Verrall and Mr Keith Stoddart, who worked extensively in
Queensland coal mines told the committee that they have experienced
considerable difficulty in getting a diagnosis and later treatment, for their increasingly
disabling respiratory problems. Mr Verrall told the committee:
I have been unwell for a good while. About 2002 is when I
started going into hospital. They said, 'You have pneumonia.' I said, 'No.'
They had the camera go down into my lungs in 2005 and that is when they said,
'You have black lungs.' They did not tell me, then; they told me much later. I
started getting the bleeding then. The first time I bled they rushed me to
Ipswich Hospital. I had five of those sick bags, there was that much blood. My
brother was sitting there and he was taking them and dropping them into the
yellow bin and giving me another one each time. I was not coughing it up, it
was like a running hose. I was in hospital, there, for a while with that.[1]
2.2
Mr Stoddart, who has had to take leave from his employment as a miner to
seek a diagnosis, told the committee:
I got a pain through my right lung. I went to see a local GP
in Bundaberg. He sent me for an X-ray and wanted a CAT scan. I said, 'I've got
to go back to work.' I went back to work for a week and I got the CAT scan up
at Emerald. It came back with fibrotic scarring. I said to the doctor up here,
'What could cause that?' and he said, 'Coaldust could cause that. You've got to
go and see a thoracic specialist.' I went down to Bundaberg to see a thoracic
specialist. I had another CAT scan that showed nodules as well, and emphysema,
because I was a smoker for a long time. There was emphysema as well as this
other stuff that this doctor did not really understand. He thought the nodules
might be cancer. He said that it is not typical of cancer. He wanted to send me
down for a biopsy on my right lung. He sent me to another specialist down in
Brisbane.
On my way to Brisbane, I had a sharp pain in my left lung. By
the time I got to Brisbane, I was struggling to breathe and in a lot of pain. I
had to do a PET scan before I could see this other doctor and get this biopsy
done. The PET scan showed activities in both lungs. He did a biopsy on my left
lung. The next day, when he said, 'There's no cancer,' I said to him, 'What
about the right lung?' He said, 'You can't do the both lungs at once, because
there is chance they will collapse. If they both collapse, you'd be in
trouble.' He did the biopsy on my left lung. I said, 'No cancer—did you look
for anything else?' He said, 'No,' I said, ‘Okay.'[2]
2.3
The difficulties experienced by coal miners like Mr Verrall and Mr
Stoddart in being diagnosed and subsequently treated, prompted the committee to
seek expert advice about the causes and progress of CWP and about how it has
been diagnosed internationally and in Australia to date. The committee also
sought information about the steps taken to date by mining companies to
mitigate CWP, about the current regulatory controls to prevent further cases of
CWP in Australia and about the Queensland Government’s response to the recent
reported cases of CWP in that state.
Coal Workers' Pneumoconiosis
2.4
The United States Centres for Disease Control and Prevention (CDCP),
quoted by the CFMEU in its submission, explains that pneumoconioses are a group
of lung diseases 'caused by inhalation of certain dusts and the lung tissue's
reaction to the dust.'[3]
The CDCP notes that the principal cause of the pneumoconioses is work-place
exposure to dust.[4]
2.5
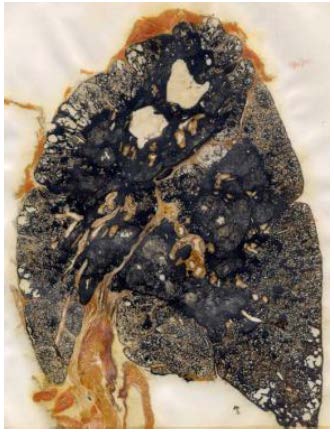
Figures 1 and 2 below show the effect of coal dust in the lungs In
Figure 1, the coal dust appears in the lung as nodules in the initial stages of
CWP.
2.6
Figure 2 shows the continuation of CWP into Progressive Massive Fibrosis
(PMF), in which large masses of fibrosis lead to:
-
severe shortness of breath;
-
moderate to severe airway obstruction;
-
severe deterioration in quality of life; and
-
associated heart problems.
2.7
Sufferers of PMF can also be vulnerable to other respiratory problems,
and as a result have a shortened life expectancy. PMF is incurable.[5]
Figure 1—specimen of a lung with CWP nodules[6]

Figure 2—specimen of a lung with Progressive Massive
Fibrosis[7]
2.8
The CDCP explains that the primary pnemoconioses are asbestosis,
silicosis, and coal workers' pneumoconiosis. Each is caused by a type of dust,
respectively: asbestos fibres, silica dust, and coal mine dust. Other forms of
pneumoconiosis can be caused by dusts such as aluminium, antimony, barium,
graphite, iron, kaolin, mica, and talc. The common factor to all types of
pneumoconiosis, according to the CDCP, is that in general these diseases take
years to develop and are caused by 'entirely man-made' conditions which
'can be avoided through appropriate dust control'.[8]
2.9
CWP is also known as 'pneumoconiosis', 'black lung', and 'coal miner's
lung'. Throughout submissions and evidence received at the committee's
hearings, these terms were used interchangeably. For clarity, the committee's
report will refer to CWP throughout.
2.10
The Thoracic Society of Australia and New Zealand (Thoracic Society) gave
a similar definition of CWP to the CDCP in its joint submission with Lung
Foundation Australia. Further the submission noted the difficulties in
diagnosing CWP:
Pneumoconiosis is a deemed disease by Safe Work Australia.
However, because it has a long latency period, often not presenting with
symptoms until many years after the worker has retired, the relationship between
the development of lung disease and its association with work may not be
identified. The risk of developing CWP is directly related to the magnitude and
duration of exposure to coal mine dust.[9]
2.11
The CFMEU submission recognised that the development of CWP is slow and only
occurs after long exposure to coal dust, noting that the disease can be
difficult to diagnose in the initial stages. Once it progresses, CWP is fatal
and there is no cure:
CWP manifests firstly as simple CWP that may produce a cough and
sputum. It can be asymptomatic – ie. No obvious symptoms. It appears in the
lungs as small (1-5mm) round nodules that appear as “opacities” on x-rays.
In a minority of cases there is calcification within the nodules.
Continuing exposure can progress to complicated CWP often
known as Progressive Massive Fibrosis (PMF) – large masses of dense fibrosis
causing severe shortness of breathe [sic], moderate to severe airway
obstruction and consequently severe deterioration in quality of life. There are
associated heart problems and it often contributes to early death.[10]
2.12
The Thoracic Society and Lung Foundation Australia explained that while
prolonged exposure to, and increased levels of coal dust will exacerbate CWP,
and will lead to the possible development of PMF, such progression can be
slowed or even prevented with early detection. It is therefore vital that regular
and rigorous screening measures are put in place, particularly at mines where
coal dust levels have risen.[11]
Coal mining and CWP
2.13
The CFMEU's submission highlights the history of coal mining and its
deadly corollary, CWP:
...the industry from its inception was extremely hazardous both
in terms of catastrophic risks and longer term health impacts. Until relatively
recently it was considered virtually inevitable that coal communities would be
blighted – that workers and their families would be poorly paid, work in
arduous and dangerous conditions, and they and their families would live in
highly polluted and degraded environments. Coal dust is intrinsic to the
hazards of coal mining – coal dust contributes to catastrophic risks through
its flammability and explosive potential along with the methane gas that is
also intrinsic to coal mining.[12]
2.14
The Thoracic Society's submission demonstrated that pneumoconiosis-related
fatalities are still intrinsically linked to mining today:
In 2013, pneumoconiosis resulted in 260,000 deaths globally.
Of these deaths, 46,000 were due to silicosis, 24,000 due to asbestosis and
25,000 due to CWP. Most of these cases occurred in the setting of poor
occupational hygiene and limited systems for dust control.[13]
2.15
The Thoracic Society noted that such is the scale of the problem; the
World Health Organisation has set down a target of eliminating pneumoconiosis
by 2030.[14]
2.16
The impacts of coal dust exposure are known to the mining industry. In
their 2011 research paper 'Dust Controls and Monitoring Practices on Australian
Longwalls' (the paper), Dr Ting X Ren, Dr Brian Plush, and Dr Najdat I Aziz of
the University of Wollongong, noted that:
Fugitive dust on longwalls has always been an issue of
concern for production, safety and the health of workers in the underground
coal mining industry globally. Longwall personnel can be exposed to harmful
dust from multiple dust generation sources. With the increase in production
created from the advancement in longwall equipment, dust loads have also
increased and this has resulted in an increase in exposure levels to personnel.[15]
2.17
The modern coal mining industry has recognised the impacts of coal dust
exposure on the health of coal mine workers. In Australia, two main practices—mitigation
of coal dust levels and protective measures for workers—are employed to protect
coal workers from exposure to coal dust. These are discussed later in this
chapter.
History of CWP in Australia
2.18
Coal mining was established in Australia by the 1830s.[16]
Australia is currently the fifth largest producer of coal in the world with
2012-13 coal production at 527 million tonnes.[17]
The majority of Australian coal is mined in Queensland and NSW, although there
are other locally significant black coal mines in Western Australia, South
Australia, and Tasmania. Brown coal is mined in Victoria.[18]
The coal industry in Australia provides direct employment for approximately 54
900 people.[19]
2.19
CWP has been a part of the coal mining industry in Australia from its
inception.[20]
But as improvements were made in mining machinery and processes, and better
protection was available for miners, incidents of CWP reduced. Government regulation
mandating screening and setting limits for the level of coal dust contributed
to what was thought to be the eradication of CWP in Australia in the 1980s.[21]
2.20
Until the first case in recent history of CWP was reported in May
2015, Australia had been hailed as having completely eradicated CWP. In other
coal mining countries like the UK and US, cases of CWP have remained stubbornly
prevalent The CFMEU
submission notes that around the world, CWP is still a major risk for coal
miners:
In most parts of the global coal industry the disease has
continued to exist despite the development of mine management systems that
reduce the risk. The United Kingdom records that between 1998 and 2004 some
570,000(!) compensation claims were made for lung disease from coal mining... In
the United States, the incidence of CWP among underground coal miners was 11.2%
in 1970–74, and 2% during 1995–99. A study by the Center for Disease Control
using 2010-11 records for open-cut miners found 2% had CWP.[22]
2.21
Regulation on the level of coal dust exposure varies from state to
state. There is no national body or legislation which determines maximum dust
exposure levels, so each state has different regulated levels of coal dust
exposure.[23]
2.22
Evidence gathered by the committee shows that there are contrasting
approaches to deal with the problem of workers being exposed to coal dust. In
some cases the focus is on measures to prevent workers inhaling the dust by way
of Personal Protective Equipment (PPE) such as face masks. In other cases the
focus is on mitigating the dust levels, for example by using water sprays
and/or ventilation to minimise workers' exposure to consistently high levels of
coal dust. These alternative approaches are highlighted below in the discussion
of the Queensland and NSW regulatory schemes.
Re-emergence of CWP in Australia
2.23
The re-emergence of CWP was reported in the 2014-15 Annual Performance
Report of the Commissioner for Mine Safety and Health, Queensland Mines
Inspectorate, in May 2015:
The first case of coal workers’ pneumoconiosis in a
Queensland coal miner in 30 years was reported this year.[24]
2.24
Between October 2015 and February 2016 a further five cases of CWP were
reported in Queensland. In April 2016, two further cases were diagnosed at Vale
Australia's Carborough Downs mine and Anglo American Coal's Grasstree mine,
bringing the total to eight cases.[25]
Queensland Health and the Queensland Department of Natural Resources and Mines
(DNRM) joint submission of March 2016 puts the number of cases officially
confirmed at six.[26]
2.25
Anecdotal evidence suggests that there may be CWP cases in other states,
including NSW, however no confirmation could be found for these cases.[27]
2.26
The sudden re-emergence of CWP prompted the Queensland Government to
conduct a review into the Coal Workers' Health Scheme (CWHS) to ascertain if
better measures need to be taken to diagnose CWP. In a media release on
14 January 2016, the Minister for Natural Resources and Mines, Dr
Anthony Lynham MP, (Minister Lynham) explained:
We have confirmed five cases of coal miner’s pneumoconiosis
in Queensland and I have asked for Queensland Health data on any other possible
cases. There’s still research to be done on the medical and workplace records,
but I suspect there are more cases to come. I am determined to get on top of
this issue to protect workers now and into the future and to be open and
transparent as we progress.[28]
2.27
Minister Lynham, announced an 'action plan' in response to the
re-emergence of CWP. The action plan has five points:
- A review to improve the existing screening system, in which coal
mine workers have chest x-rays when they start work, then at least every five
years until retirement. The review is being conducted by Professor Malcolm Sim
from Monash University. Professor Sim's interim report was provided to the
Queensland Government in March 2016, and published on 8 April. His detailed
final report will be handed down by the middle of 2016.
- Taking action on coal mines exceeding regulated limits on dust levels.
Minister Lynham's media release noted that 'Coal inspectors are working closely
with all of Queensland's 12 operating underground coal mines, including those
with coal dust issues related to longwall mining techniques.' Further, 'of
Queensland's 12 operating underground coal mines, only one is exceeding dust
limits now. Eight mines over the past 12 months have been directed to either
improve monitoring or bring respirable dust levels back into compliance.
Directives will remain in place until mines inspectors are satisfied that mines
can stay within the regulated level.'[29]
- Improving
how information is collected and used to ensure cases are not missed.
- Investigating regulatory changes as part of the mine safety
legislation review already underway. The Minister's media release explained
that the updating of legislation 'will include a focus [on] what changes are
required to ensure underground coal dust is kept at safe levels.' At the
committee's public hearing, Mr James Purtill, Director-General, DNRM, told the
committee that work is continuing on the detail of the regulatory changes and
the DNRM aims to have amendments for the Queensland Government to consider
later in 2016.[30]
- Placing the issue on the agenda for the National Council of Mining
Ministers. Minister Lynham noted that he had written to the Minister for
Resources, Energy and Northern Australia, Mr Josh Frydenberg MP as head of the
Council.[31]
2.28
The Queensland Government and the coal mining company Vale Australia,
engaged United States radiology expert Professor Robert Cohen to examine
current coal miners' x-rays to improve current screening arrangements for CWP.
An examination of former miners' x-rays was also part of Professor Sim's review
for the Queensland Government.
2.29
With examination of x-rays moving to the US, and new cases of CWP being
diagnosed, confidence in the CWHS screening process declined significantly.[32]
This also led to criticism of the training Australia radiologists had received
in diagnosing CWP, as the US B-Readers[33]
were reporting to International Labor Organisation (ILO) standards; a reporting
standard not widely used in Australia.[34]
2.30
The Royal Australian and New Zealand College of Radiologists (College of
Radiologists), responding to criticisms that too few Australian radiologists
had the necessary training to diagnose CWP,[35]
published a list of 36 'clinical radiologists who are available to report on
chest x-rays to screen Australian miners for CWP, in line with the ILO
Classification.'[36]
This list was published on 4 March 2016.[37]
2.31
The College of Radiologists detailed the history and methodology for ILO
reporting and its current advice to members about ILO reporting on CWP cases:
The International Labour Organization (ILO) Classification of
Radiographs on Pneumoconioses which was created in the 1980s has not been
widely used recently to classify radiographs for CWP in Australia. Clinical
radiologists have instead used standard reporting templates for diagnostic
imaging when reporting on CWP, which was appropriate given that CWP had not
been seen in Australia for the last twenty years.
This ILO classification works by using the standard set of
radiographs as a point of reference that allows for consistent reporting of
pneumoconiosis and other interstitial lung diseases. The patient’s radiographs
are classified after they are compared with the standard radiographs using a
step-by-step method to describe the lesions. The results obtained are then
recorded in a systematic fashion.
RANZCR has advised our members that clinical radiologists
should only report on screening chest radiographs for CWP if they:
-
have experience in reporting screening radiographs for
pneumoconiosis,
-
are familiar with the ILO Classification and willing to report
using the Classification, and
-
have sufficient caseload of referrals to maintain their
competence in this area.[38]
Mitigation of coal dust levels
2.32
Professor Malcolm Sim from Monash University is leading the review team
examining the CWHS, as part of the five point action plan announced by the
Queensland Government. In Professor Sim's interim report, released on 8 April
2016, he explains that mitigation of coal dust levels begins with setting
exposure limits, which he says are:
...measured as mean air concentrations over 8 hours (i.e. an
8-hour time weighted average (TWA)). If the shift is normally 12 hours for 5
days (i.e. longer than 40 hour per week) the mean exposure must be compared to
a proportionally reduced limit (e.g. 8/12). This is because for coal dust and
silica, increased risk is associated with cumulative exposure rather than
exposure intensity.[39]
2.33
Professor Sim's report explains that coal dust exposure limits are set
so as to limit the risk of workers developing CWP:
In 1986, a NIOSH-commissioned [National Institute for
Occupational Safety and Health] study carried out in the UK, showed that for
coal with a carbon content of 86.2% and exposure at 2 mg/m3, the 40‑year
risks were 1.15% for PMF and 7.75% for CWP; for coal with a carbon content of
83% and exposure at 2 mg/m3, the risks were 0.71% for PMF [Progressive
Massive Fibrosis] and 6.49% for CWP; and for coal with a carbon content of 83%
and exposure at 1 mg/m3 the risk was 3.4% for CWP. These risks were
estimated based on CXRs [chest x-rays] taken during employment and are
calculated for a 58 year-old miner. The study did not examine risks after
retirement.
A CWP prevalence study of US bituminous coal miners estimated
likely exposure based on measured data extrapolated to earlier years.
Prevalence of CWP category 1+ (small opacities) was related to cumulative dust
exposure; for individuals with <30 mg-year/m3 prevalence was
<5%, but prevalence was 30% for the group with exposure >110 mg-year/m3.
On the basis of these data, miners of lignite and sub bituminous coal who work
for 40 years at 2 mg/m3 were predicted to have a 1.4% risk of having
PMF on retirement and 14% were predicted to get CWP ILO category 1+. Miners of
harder bituminous coal were expected to have higher risks, with over 20%
predicted to get CWP category 1+.[40]
2.34
At a limit of up to 3 mg/m3 Professor Sim noted that
Australia and New Zealand have 'the highest value listed for respirable dust'.[41]
2.35
Disturbingly, Professor Sim found that:
These data suggest that 30 years of exposure at the current
Australian occupational exposure limit of 3 mg/m3 respirable dust would
be likely to result in 15–25% prevalence of CWP depending on the hardness of
the bituminous coal.[42]
2.36
The Queensland Resources Council, a peak industry association which
represents commercial developers in Queensland's minerals and energy resources
sector, writing on behalf of its member companies stated that:
The industry invests significant effort across a range of
professional disciplines to proactively manage the respirable coal dust
exposure of its workers. Workers do not simply work unprotected and exposed in
dusty environments underground. There are a range of controls beyond the
regulated exposure standard that further mitigate their exposure to dust.
Regulation alone does not work.[43]
2.37
The Queensland Resources Council's submission listed a number of
techniques used in the mining industry to control dust:
-
Prevention and Control – Minimizing the production of dust by
mining machines
-
Dilution – Use of adequate ventilation
-
Suppression – Use of water sprays and other techniques e.g.
enclosure of dust sources
-
Changing the operator's position – Use of remote control
operation of certain machinery
-
Personnel Protection – Use of dust respirators[44]
2.38
The Queensland Resources Council's submission stated in relation to this
list of controls that:
Every one of these controls reduces the risk of dust exposure
and would be present/practised in underground mines as detailed in their
approved safety and health management systems. It is in the interests of the
industry and its workers that it continues to strive to achieve improvements in
these control measures.[45]
2.39
That coal dust exposure, an inevitable part of coal mining, causes CWP,
was not disputed by any witnesses. However, evidence taken by the committee
during its public hearings contradicted the Queensland Resources Council's
submission in terms of the extent to which mining companies were working to
mitigate dust levels in mines.
Protective measures for workers
2.40
Mining company Vale Australia submitted that it had taken 'proactive
measures' to mitigate dust levels at its Carborough Downs mine, 'including
application of additional engineering solutions, system improvements, [and]
operational modifications', following the reporting of CWP cases.[46]
2.41
Other measures taken by Vale Australia included:
-
review of employees' x-rays by Dr Robert Cohen in the United
States;
-
communication with workers, including briefings and an address by
Dr Cohen;
-
dust monitoring including increased frequency of monitoring, real
time monitoring and analysis of operator positioning; and
-
continued focus on the PPE including education on the correct use
of PPE, implementing a clean shaven policy, face fit testing, and mandated
Positive Air Powered Respirators (PAPR) for employees at high risk of dust
exposure.[47]
2.42
The distribution of PPE by coal mining companies, particularly
disposable face masks, was discussed at the committee's hearings. The evidence put
before the committee showed a major contradiction between the views of the
mining companies and the experiences of the coal mine workers as to the
availability and efficacy of face masks. This issue is discussed further in
Chapter 3.
Screening for CWP
2.43
The Queensland CWHS is said to protect
'the health of Queensland coal mine workers [in that state] by ensuring they
undergo periodic health assessments.'[48]
The CWHS is established by the Coal Mining Safety and Health Regulation 2001.[49]
2.44
Under the CWHS, pre-employment health assessments are mandatory for
potential mine workers and are periodically required by the employer's
Nominated Medical Adviser (NMA). There is a minimum requirement that they must
be conducted at least once every five years.[50]
2.45
NMAs are pivotal in the CWHS and are required to:
-
conduct the health assessments required for mine workers;[51]
-
order chest x-rays–the NMAs must provide all relevant information
about the worker and their exposure to coal dust to radiologists;[52]
-
provide copies of the assessment to the relevant parties
(workers, DNRM), and to the worker's employer;[53]
and
-
store health assessment data, x-rays, and x-ray reports.[54]
2.46
If an employer receives notice that the level of risk to a miner's
health has increased, a copy of the notice must be provided to the NMA so that
the worker's exposure can be monitored.[55]
2.47
Importantly, NMAs are appointed and renumerated by mining companies. The
DNRM has no role in the appointment of NMAs. There is no specific training
required for NMAs other than current registration with the Australian Health
Practitioner Registration Agency (AHPRA) as a medical practitioner.[56]
2.48
Other than setting down some screening requirements, the CWHS places the
onus on mining companies to make provision for miners' health. The current
Queensland Government review of the CWHS (the Sim review, discussed above and
in Chapter 3) has identified a number of problems with the CWHS, including the
fact that results of screening are not communicated to workers.
2.49
The committee heard concerns that the coal miners' x-rays taken under
the CWHS had not actually been examined by radiologists. This issue is
discussed further in Chapter 3.
Queensland regulation
2.50
Aspects of Queensland mine safety and health are regulated under the
following acts:
-
Mining and Quarrying Safety and Health Act 1999 (Qld) (with
the Mining and Quarrying Safety and Health Regulation 2001); and
-
Coal Mining Safety and Health Act 1999 (Qld) (with the
Coal Mining Safety and Health Regulation 2001).
2.51
The Coal
Mining Safety and Health Regulation 2001 (Qld) provides that:
- A coal mine's safety and health management system must
provide ways of ensuring—
- each coal mine worker's exposure to respirable dust at
the mine is kept to an acceptable level; and
- the worker does not breathe an atmosphere at the mine
containing respirable dust exceeding an average concentration, calculated under AS 2985, equivalent to the following for an 8-hour period—
- for coal dust—3mg/m3 air;
- for free silica—0.1mg/m3 air.[57]
2.52
The Coal Mining Safety and Health Regulation 2001 (Qld) also provides
for the CWHS as outlined above.
2.53
A mine's compliance with the regulations is monitored by Mines
Inspectors, which is a part of the DNRM. The Commissioner for Mine Safety and
Health (also a part of the DNRM) monitors mine health and safety and reports to
the Minister and Parliament on these issues. Monitoring of mining industry
compliance can include a 'review of the dust monitoring data and visual
inspection of the work areas at the mine'.[58]
2.54
If mines are non-compliant with regulations on dust levels, the Mines
Inspectors can issue a legal Directive to a mine operator. Continued
non-compliance can result in penalties such as suspension of production.[59]
The committee comments on the operation and issuing of these Directives in
Chapter 3.
NSW regulation
2.55
Unlike the Queensland regulatory scheme, the NSW regulatory scheme is managed
by an entity separate to the NSW Government. The Coal Industry Act 2001
(NSW) creates the entity, NSW Coal Services which is jointly owned by the NSW
Minerals Council and the CFMEU.
2.56
NSW Coal Services has a number of statutory functions under the Coal
Industry Act 2001 (NSW). These include:
-
providing occupational health and rehabilitation services for
workers engaged in the coal industry, including providing preventative medical services,
monitoring workers' health and investigating related health matters;
-
collecting, collating and disseminating accident and other
statistics relating to the health and safety of workers engaged in the coal
industry;
-
referring matters relating to the safety of workers engaged in
the coal industry, as it thinks fit, to the regulator within the meaning of the
Work Health and Safety (Mines) Act 2013 (NSW);
-
reporting to the Minister as it thinks fit, or when requested by
the Minister, on matters related to the health or welfare of workers engaged in
the coal industry, or on any other matter arising out of its functions;
-
monitoring, promoting and specifying adequate training standards
relating to health and safety for workers engaged in the coal industry; and
-
monitoring dust in coal mines.[60]
2.57
NSW Coal Services is part of a 'collaborative model' which includes
industry, the NSW Government, employers and mine operators, unions, and mine
workers. The emphasis of the model is on prevention of injury and disease.[61]
Various business units of NSW Coal Services carry out the statutory functions.
2.58
NSW Coal Services is independent of industry and this allows it to
rigorously monitor coal dust levels, as Ms Lucy Flemming, CEO of NSW Coal
Services explained:
The dust requirements in New South Wales are pursuant to the
regulation which prescribes monitoring requirements for respirable dust,
including specific locations and frequencies of that dust monitoring. It is
actually very highly regulated. That regulation also directs us to be
independent of the mine and we must be licensed by the New South Wales
Department of Industry, Division of Resources and Energy. If we do measure any
dust exceedences, there must be resampling and corrective action taken.
To help us do all of that there are two government gazetted
orders which are both administered by Coal Services. They are order 40, which
is the longwall dust abatement approval that we must approve plans for dust
abatement on longwall, and order 42, which is the mandatory monitoring and
prescribed exposure limits. An important thing to note specifically in order 42
and dust monitoring that per the New South Wales health and safety mines
regulation 2014—a fairly new regulation—mineworkers are sampled regularly.
Order 42 requires that all of the crews in each separate work area of the mine
identify any systemic issues that may result from mining practices in a
particular work team. So every panel on every shift over a period is monitored.
What happens with those results? They are sent to the mine operator, they are
sent to the Inspector of Coal Mines and they are also sent to the industry
safety and health representative.
If there is a failed result, the mine manager informs that
person who was sampled, so the actual miner where this has occurred, and there
is an obligation under the New South Wales Work Health and Safety (Mines) Reg
2014 to conduct a review and take corrective action. The whole crew is
resampled and we look for any systemic issues that may be occurring and
recommend corrective actions—again, working collaboratively with the mines
management team to rectify any issues.[62]
2.59
A further mechanism to ensure review of dust sampling is the Standing
Dust Committee:
This is a subcommittee of the Coal Services board. It meets
bimonthly and maintains an overview of the results of the dust sampling
program. All relevant industry participants sit around the table. The industry
representatives that we have on this table include the department and the
inspectorate, the industry safety and health representative, health services
experienced staff, the employer and operator representatives and a couple of
independent industry experts and workers.[63]
2.60
Ms Flemming told the committee that the proof of the success of the NSW
Coal Services model has been in its reduction of injuries:
...a reduction in injuries that have been reported of over 75
per cent in that period, which is a large reduction. Back in 2001-02, probably
one in four people were injured, and in an underground mine, that was more like
one in three. Now we have less than six per cent; currently it is just on 5.5
per cent. Fewer than six people per hundred over that period, which to us is a
great example of that model actually working and delivering a safe workplace
and healthy workforce for the coal mining industry.[64]
2.61
The Coal Services Occupational Hygiene business unit conducts dust
monitoring:
The Coal Services Occupational Hygiene team include a broad
and multi-discipline skill set incorporating hygienist, specialist laboratory
technician and coal industry experienced inspectors. In Coal Service's view,
being an effective licenced provider requires more than simply applying
personal dust monitors...The Coal Services inspectors are typically experienced
in underground and mining practitioners...Our inspectors travel underground with
the mining crew to conduct the dust monitoring, observe operational practices,
audit control measures and provide on the spot guidance and education to the
underground miners literally "at the coal face".[65]
2.62
The CS Health business unit provides health services, including x-rays
and chest screening. The CS Health screening program includes a pre-employment
medical, a regular (three yearly) medical, and chest x-rays every six years for
miners with a history of possible hazardous dust exposure. All x-rays are
reviewed by a radiologist and any abnormalities are referred to an appropriate
medical professional for further investigation.[66]
Committee view
2.63
The committee's examination of issues which background the re-emergence
of CWP has identified the following key issues:
-
CWP has returned to Australia. There are currently eight
confirmed cases, but that number is very likely to rise.
-
The best way to prevent coal dust exposure which leads to CWP is
in dispute. Some prioritise prevention of high coal dust levels, while others prioritise
individual worker protection.
-
Screening for CWP and other coal dust related conditions is also
the subject of debate and approaches vary from state to state.
-
Finally, whether Australia has the expertise, and the health
infrastructure, to properly diagnose CWP and support those with the disease will
be key to how mining states move forward.
2.64
The re-emergence of CWP in Australia after such a long period is deeply
concerning. While mining production in Australia creates export earnings in the
tens of billions of dollars, those who are literally at the coal face are given
a death sentence in the form of incurable CWP. The committee believes that
action now is essential if further cases of CWP are to be prevented in the
future. The remainder of the report provides evidence and arguments to support
this conclusion and recommends action which will help eradicate the spectre of
CWP in Australia.
Navigation: Previous Page | Contents | Next Page